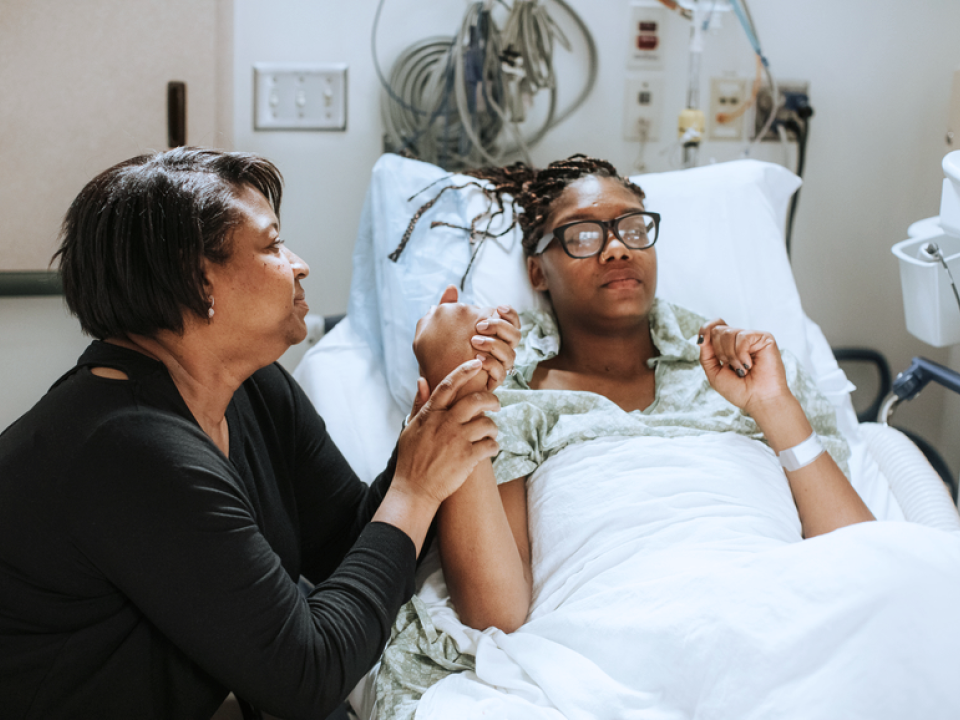
The possibility of developing breast cancer can feel daunting. While the likelihood of diagnosis varies depending on your age, family history, breast density and more, one fact is certain: early detection from breast screenings can save lives.
“I was diagnosed on my 35th birthday, and the doctor didn’t want to originally give me a mammogram,” says Bridgette Hempstead, a breast cancer survivor and patient advocate.
Anyone with breasts has the potential to get breast cancer, but Black women are diagnosed at earlier ages than white women.
“Black women are diagnosed with breast cancer about four years earlier than white women, around age 59 versus 63,” says Janie Lee, MD, professor of radiology at the University of Washington School of Medicine and director of Breast Imaging at Fred Hutch Cancer Center.
But not enough Black women are getting screened early enough — or at all.
When should you start breast cancer screening?
For context, most cisgender women can choose to get their first mammogram between ages 40 and 44 if they wish to do so, or earlier if they are at high risk of developing breast cancer. General breast cancer screenings are recommended to start at age 40 and continue at least every other year.
Transgender women who are over the age of 40 and have undergone hormone replacement therapy (HRT) for five or more years should also consider getting a mammogram around this time.
In addition to the higher rates of diagnosis at an earlier age, the breast cancer mortality rate is 39% higher among Black women. If breast cancer is a potential threat for all people with breasts, why are Black women dying at higher rates?
What we know about breast cancer in Black women
According to the American Cancer Society, breast cancer is the most commonly diagnosed cancer among Black women. It’s the second-most common cause of cancer death in Black women, right behind lung cancer. Black women are also twice as likely to be diagnosed with triple negative breast cancer — a more dangerous tumor with fewer effective treatment options.
“Twenty-two percent of breast cancers in Black women are triple negative, compared to 10 to 12% of women in other races,” Lee says. “If you’re a Black woman, getting your screening mammogram could be crucial to catching an early breast cancer and treating it.”
So, if we have these statistics, why aren’t more Black women getting screened for breast cancer? The answer is a bit more complex than it seems.
Medical anxieties in the Black community
Historically, Black Americans have experienced medical abuse. The most well-known example is the infamous Tuskegee experiment, a decades-long study led by the United States Public Health Service and the Center for Disease Control and Prevention.
From 1932 to 1972, doctors observed the effects of untreated syphilis on Black Americans and withheld medical care for it even after a treatment for the disease was found in 1947. Over 100 Black Americans died during this study, which resulted in widespread mistrust of medical professionals throughout the Black community.
“Because of Tuskegee and other horrific moments that have happened to the Black community, the fear is real,” says Hempstead.
One thing that’s helped? Seeing a doctor of the same race. Adewunmi Nuga, MD, a primary care doctor at UW Medicine Primary Care – Kirkland, says studies have found that counties with a higher percentage of Black doctors also showed an increase of life expectancy for Black people.
“We also need more diversity in medical studies and research,” says Nuga.
How to encourage more Black women to get screened
Unfortunately, the obstacles Black women face are not limited to anxiety and mistrust of medical professionals. Here are some other challenges, paired with actionable suggestions from our experts.
Navigate the barriers
If you live in King County and lack of insurance coverage is preventing you or a loved one from getting a necessary screening, you can call Seattle King County Public Health. They can connect you to the Breast, Cervical, and Colon Health Program, which will help you get coverage for your first mammogram. If you are diagnosed with breast cancer, your care could be entirely covered. Statewide resources are also available for those who don’t live in King County.
And there are options other than going to a doctor’s office. The Fred Hutch Cancer Center has a Mobile Mammogram Van that travels to different cities in King and Snohomish counties to help women get breast cancer screenings closer to where they live and work. In the last year, the Mobile Mammogram Van performed over 5,000 screenings, with an additional focus on underserved areas.
Promote self-advocacy
Regardless of how thorough a doctor may (or may not) seem, it’s essential for Black women to advocate for themselves during their patient visits.
Nuga says it can be discouraging for patients to feel dismissed and not receive the care or information they need, but that persistence will pay off in the long run.
“Sometimes it can take more than one visit to address all the issues, which makes it important to see things through with follow-up appointments,” she says.
Come to your appointment with a list of questions you want to ask about your breast health. Do you feel like something is off and a doctor won’t address it? You, as the patient, have the right to push back.
“The younger you are, the harder it is to be heard,” Hempstead says. “When clinics and doctors ignore signs of breast cancer in Black women, it’s an early death sentence. We have to advocate and fight for our own lives.”
Provide low-stress options
At the end of the day, getting screened is an act of self-love and a form of self-care. If you’re wanting an accountability partner or looking for ways to make the appointment less stressful, Hempstead recommends bringing a sister, friend, mother or other loved one to the appointment. You may even consider scheduling appointments together and making a day out of it by celebrating your bravery by having an after-appointment lunch date or exploring the city when you’re done.
“Screening is a part of a program of self-care and wellness. It’s a way of helping women stay healthy by finding a cancer when it’s early, and before symptoms develop if the cancer is present,” Lee says.
If you are a Black woman and you’re hesitant to get screened for breast cancer, that’s a completely normal and justified feeling. But in the words of Hempstead, “It’s an exam that could find an early-stage cancer and give you the opportunity to continue to love on your loved ones and live your life. There is life after breast cancer.”
This article was originally published Oct. 25, 2021. It has been reviewed and updated with new info.

 Healthy ideas for your inbox
Healthy ideas for your inbox