Few things are more personal than figuring out the birth control method that works best for you. After all, finding the perfect fit is essential — you want to ensure that your ultimate choice plays well with your lifestyle, health and finances.
Luckily, we people with uteruses have many options (though fingers crossed that those long-awaited male contraceptives will eventually grace us with their presence). If you’re the kind of person who prefers to pop a pill every day, there are lots of hormonal birth control pills that will fit the bill, whereas condoms are useful “on-demand” options for someone looking for protection from both STDs and unwanted pregnancies. And for those looking for a more long-term, hands-off solution, an IUD (or intrauterine device) might be a perfect fit.
However, there is still some confusion about what exactly IUDs are and how they work. This is why we’re here to offer up facts, information and everything else you need to make an educated decision.
How does an IUD work?
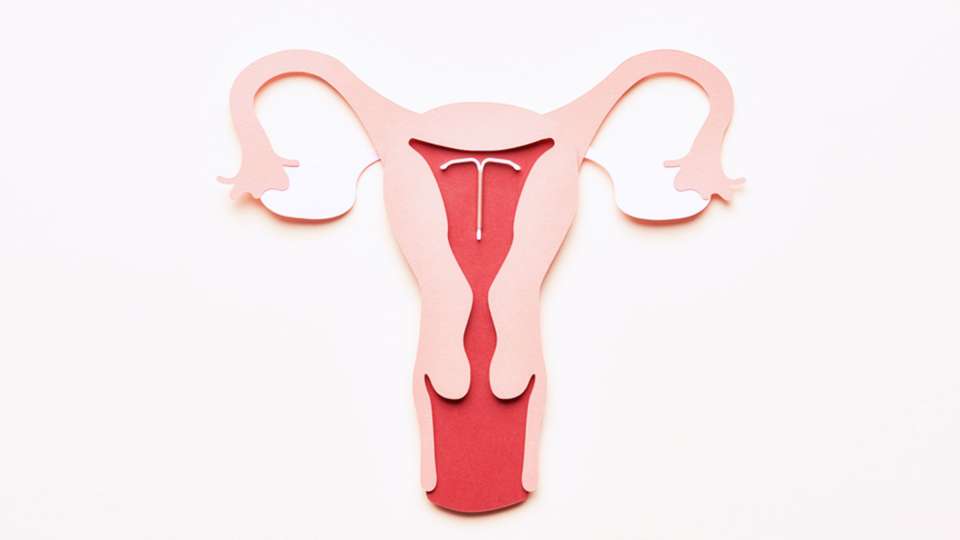
Simply put, an IUD is a tiny T-shaped device inserted into your uterus by a medical professional to help prevent pregnancy. There are two options: copper or hormone-based — each offering a slightly different experience for the user.
The copper IUD is:
- Referred to as ParaGard or “nonhormal IUD”
- Wrapped in copper wire, which is toxic for sperm and eggs
- Effective for at least 12 years
The hormonal IUD is:
- Either Mirena, Kyleena, Liletta or Skyla
- Made with the hormone progestin, which is similar to the progesterone that we naturally make
- Effective because it thickens the mucus in the cervix to prevent sperm from reaching an egg and thins the lining of the uterus
- Effective from three to eight years (depending on the kind)
What are some of the most common myths about IUDs?
As we mentioned, there are plenty of mixed feelings about IUDs — mostly because people just don’t really understand them.
According to Dr. Lyndsey Benson, an OB-GYN specializing in complex family planning at UW Medical Center – Montlake, the following are the most common myths that she encounters when discussing IUDs with patients:
MYTH: IUDs can cause abortions
IUDs primarily work by preventing fertilization, so the sperm cannot meet the egg. For example, copper acts as a spermicide, and the progestin hormone in hormonal IUDs causes thickening of the cervical mucus so the sperm cannot get through the cervix. There is no evidence that an IUD will interrupt an implanted pregnancy.
MYTH: IUDs can cause infertility
This concern pops up often, which is why Benson wants to emphasize that IUDs do not increase the risk of pelvic infections or infertility. Also, since they aren’t permanent, you can have your IUD easily removed by a nurse or doctor whenever you choose, and you can even get pregnant soon after.
MYTH: IUDs cause ectopic pregnancies
“Since the overall likelihood of pregnancy is much lower, the risk of ectopic pregnancy with an IUD, in general, is extremely low, and much lower than the risk of ectopic pregnancy when not using any contraception,” Benson says.
Though the chances are very slim that you’ll become pregnant while you have an IUD in place (less than 1%), if you do, the likelihood that it is an ectopic pregnancy is increased.
MYTH: It is not healthy to miss menstrual periods with a hormonal IUD
Also untrue! Yes, hormonal IUDs help thin the lining of the uterus, leading to lighter periods (or even no periods at all), but this doesn’t cause any harm to your body. And it’s reversible after the IUD is removed, meaning your normal periods will come right back (whether you like it or not).
The benefits of an IUD
There are plenty of benefits that come with using an IUD — one of the most important being that you don’t have to think about it once it’s been inserted. Plus, as mentioned above, they’re one of the most reliable birth control methods (over 99% effective) and can last anywhere from three to 12 years depending on the type you decide on.
Another plus? “Both copper and hormonal IUDs can be used as emergency contraception when inserted within five days of unprotected intercourse,” says Benson. Hormonal IUDs also help protect against uterine cancer.
Hormonal IUDs generally make your menstrual periods lighter — and sometimes even make them go away completely — although some people do experience irregular bleeding or spotting for a few months after placement. It’s also important to note that the hormone-free copper IUDs can have the opposite effect, causing heavier periods and more cramping (but no hormones!).
Another thing to consider: people are often scared of the IUD insertion process because they’ve heard endless horror stories (we’re looking at you TikTok). Honestly, it’s different for every person, with some folks finding it only mildly irritating, and others feeling very uncomfortable. Ultimately, it’s important to be upfront with your doctor, ask as many questions as you want about pain relief options and be communicative about any pain you are experiencing.
The good news? The whole process generally takes around 10 minutes — so you should be in and out of the office before you know it.
The real issues to look out for when it comes to IUDs
Of course, nothing is perfect. There are some side effects that you’ll want to be aware of when you’re using an IUD, the most common one being a change in bleeding, which usually means spotting between periods or a heavier or lighter flow.
Also, if you're having an IUD placed right after you’ve given birth, you should be aware of the risk of an IUD expulsion (when the device either partially or completely falls out of the uterus) — though this is not a super common occurrence. Doctors often recommend getting an IUD placed immediately after delivery, which though convenient, can increase the risk of IUD expulsion.
Cramping, pain, abnormal bleeding or discomfort during sex can all be symptoms of an IUD expulsion — and signs that it’s time to schedule an appointment with your OB-GYN. At that point they can give you a pelvic exam or an ultrasound to figure out what the deal is.
The (tiny) chance of a uterus puncture
IUD perforation, when the device punctures the uterus or cervix, is another unlikely, but possible, complication that can arise from having an IUD inserted. This recent study, led by UW Medicine’s Dr. Susan Reed, focuses on women who had an IUD placed in the year after giving birth and women who had one placed while they were breastfeeding.
According to the study, the risk of perforation was higher for breastfeeding women and women who had their IUD inserted between four days and six weeks postpartum. Perforation rates were lower if the IUD was inserted right after delivery, over a year later or in women who hadn’t delivered babies.
Though the study is intriguing, it’s important to understand that these complications are not common (in fact, the risk of uterine perforation is 1 in 1,000) and that IUDs remain a reliable and beneficial form of birth control for people all over the world.
In conclusion
Overall, for many people the perks of IUDs will outweigh the risks. Which is why it shouldn’t be too surprising that they have the highest “user satisfaction” when it comes to birth control methods. After all, once you've had your IUD inserted, you can get right back to your life — knowing that one magical little device is doing the hard work of not having a baby for you.

 Healthy ideas for your inbox
Healthy ideas for your inbox